What’s In The Water You’re Swimming In?
By Kerri Cooke
The return of sky-high humidity and heat indexes at 100 degrees means it is time for a beach trip.
Summer months are peak beach season because not only are people trying to cool off, the ocean water is warm enough to comfortably enter. However, before you go to the beach, make sure you are informed about the illnesses that can occur when you come into contact with its salty water.
While it might be unusual to get sick after visiting the beach, it is not impossible. Most illnesses are short lived and minor, but there are a few that can be dangerous. And beach-borne illness are more common in people who are just getting over an illness or people with pre-existing conditions, such as cirrhosis, diabetes, cancer and obesity.
Here is a guide on the pathogens that can live in the water and how to protect yourself.
Enterococci
Enterococci is the bacteria you will hear about most when it comes to beach cleanliness and safety, especially since it plagues many beaches in Southwest Louisiana and Galveston.
Water becomes contaminated with high levels of the bacteria when heavy rains occur and wash sewage and fertilizer into local waterways. Levels are also increased by animal and bird waste and by adults or children who have not sufficiently cleaned themselves.
According to Dr. Lacey Cavanaugh, the regional medical director for the Louisiana Dept. of Health, bacteria grows quicker in hot weather. An absence of rain can also lead to high levels in beach water. If there is no water to dilute the colonies of bacteria that have grown, that can be problematic as well.
Enterococci naturally occur in the digestive system of humans and animals, so it is present in feces as a waste product. Usually you will see warning signs set up on beaches when there is a high level of bacteria. Beach water is tested for it regularly. Most of the time, the signs are just a warning to beachgoers that they enter at their own risk. However, if the levels of enterococci are high enough, officials may end up closing the beach.
If a person has an open wound or their immune system is compromised, they might want to avoid swimming. Infections and diarrhea can occur. Rashes can also occur. For healthy children, adults and pets, the main thing is to avoid swallowing ocean water.
Sea Lice
Sea lice is a misleading name for the tiny little creatures that sting beachgoers, creating an intense itch. Actual sea lice are parasites that feed on salmon. But the beach pests called sea lice are thimble jellyfish and a species of sea anemone that are in their larval stages.
These pests were originally named sea lice by natives of Florida in the 1950s when they got rashes after swimming on beaches. They couldn’t see the perpetrators, so sea lice must’ve seemed like an appropriate term. The correct term is actually seabather’s eruption.
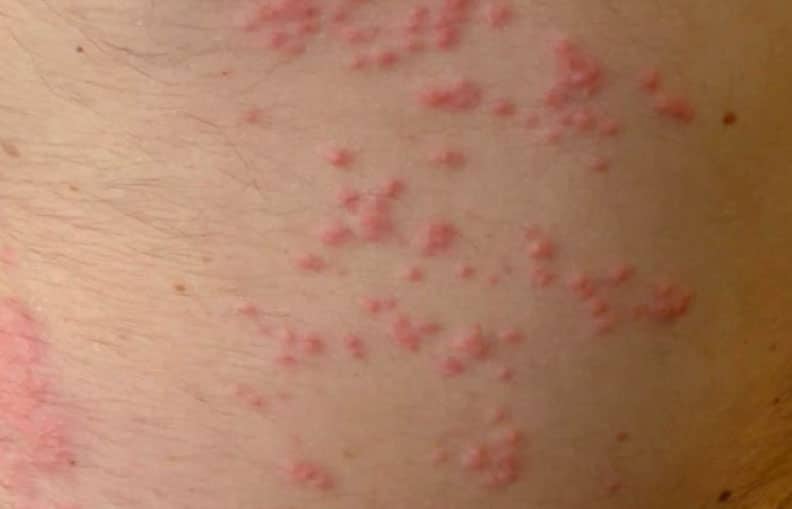
Seabather’s eruption is caused when translucent, tiny larva sting the skin and release toxins. The toxins then create a small red rash. These sting marks can be all over the area where tight garments were worn.
Sea lice are most prevalent from March to August. Outbreaks have worsened over the past few years, possibly due to warmer water. Thimble jellyfish larva originate around Mexico and in the Caribbean Sea. Their dispersal is affected by ocean currents. They tend to be more regular and widespread in Florida than in areas along the Gulf Coast or the Eastern Seaboard. However, sometimes sea anemone larva pass along the northeastern states and cause an outbreak when their dispersal happens to coincide with summer months.
You would think that wearing more clothing at the beach would help prevent stings, but the less material one has on the better. It is when the jellyfish or sea anemone get trapped within a swimsuit that problems begin.
If any pressure is applied to the larva, they will feel threatened and release their toxins. If you get out of the water and recline on a beach towel, that is a recipe for sting city.
If you are a victim of sea lice, it is important to shower as soon as possible. But make sure and remove your swimsuit first. If you don’t, the sea lice are still in contact with you and will sting more. Sea lice can also accumulate in hair, so make sure you give your tresses a good rinse as well.
It is possible you might not feel the stings until a day later when they cause an allergic reaction. Other people will notice a prickling sensation while still in the water. The rash can last for up to a week or two.
It is important to properly treat your swimsuit if it’s been infested with sea lice. Hang-drying your suit is not enough. Even washing it might not be enough. After washing, make sure and dry the suit in the dryer to kill off any sea lice still alive.
Treat your itchy rash with hydrocortisone cream, calamine lotion or antihistamines. Those who have had a previous reaction are more likely to have another one. If the allergic reaction gets too bad or causes other symptoms, then see a doctor. But, once again, severe symptoms are rare. Sea lice are mostly a cause of discomfort and pose little danger.
While sea lice seem to be less of a problem nearby, they can still show up. Last year, there was a report of sea lice in Holly Beach.
Wearing sunscreen is one method, besides staying out of the water, that seems to deter sea lice from stinging. Be sure to stay tuned to local news to make sure no outbreaks are reported before heading to the beach.
Swimmer’s Itch
Swimmer’s itch is also an allergic reaction. However, this allergic reaction is due to a parasite. The larva of a flatworm that lives in both snails and seagulls are the cause of this skin condition. The rise in swimmer’s itch usually corresponds with increasing water temperature and migrating birds.
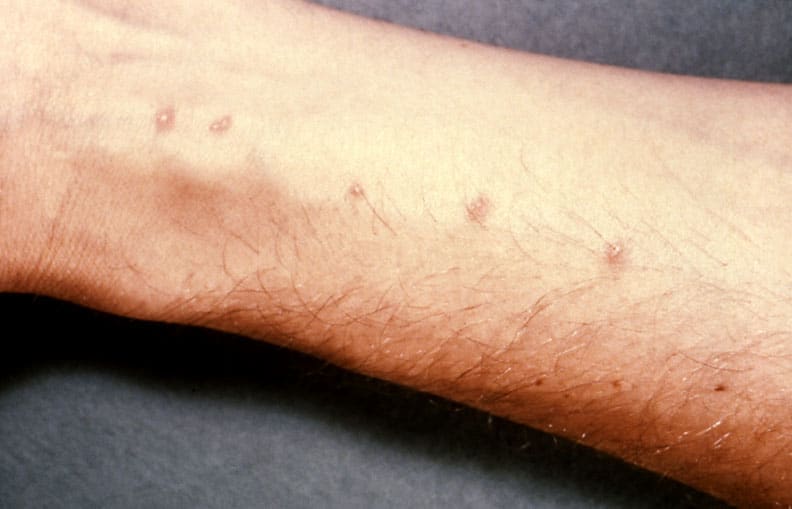
The first host of the parasite is a snail. The parasite reproduces in the snail and then leaves, looking for its next host. At the beach, that would be most likely a seagull. However, the parasite can get confused and try to use a human as its host. When the larva enter the skin, they die. But they still cause an allergic reaction that can create pimple-like bumps on the skin, just without the puss. You won’t see the signs right away — most likely the next day.
I have experienced swimmer’s itch after swimming at Galveston Beach on two different occasions. Oddly enough, it has never caused me to itch, but the numerous papules covering my face and chest were mortifying to my vanity. It took five days or so for my skin to clear. While it is said previous infection can worsen symptoms if re-infected, that wasn’t the case for me. However, it was a year or two between reactions.
If the parasite invades a seagull, it will lay eggs inside the seagull’s digestive system. Then when the seagull defecates, they are dumped into the ocean, thus recreating the vicious cycle.
Shallow water tends to have a higher number of these parasites than deep water. Some scientists say that the parasites leave their snail hosts in greater numbers on sunny days and in the morning hours.
If you are a victim of swimmer’s itch, the papules will last for a few days. The itch can be treated with antihistamines, Epsom salts, baking soda or oatmeal.
Stomach Bugs
Lots of vomiting, diarrhea and a fever are not what you want to leave the beach with. But you can contract stomach flu at the beach.
Common stomach flus you could come into contact with are the norovirus, salmonella poisoning and E. coli poisoning. All three of these ailments come from one source: feces.
The virus and bacteria can live in the sand and water on beaches after animal or human waste drifts in after recent rainstorms, or perhaps in a soiled diaper someone didn’t properly dispose of.
Avoid touching your face while at the beach; try not to accidentally consume seawater; and wash your hands when you leave. Once again, if you happen to contract the stomach flu, it is usually of short duration and does not require medical attention unless symptoms become severe.
Algae Blooms
When you think of algae, the first thing that likely comes to mind is the thick, green masses in local ditches and waterways. This type of algae is a nuisance but relatively harmless. However, there are forms of algae that are more dangerous to humans and marine life.
The most notable cases of dangerous algae blooms along the Gulf Coast are in Florida. Almost every year there is an outbreak of algae known as a red tide.
Red tides consist of large populations of algae that cluster in ocean water due to various reasons. Certain nutrients have a high correlation with a rise in the density of red tides. Nitrogen and phosphorus are fuel for this type of algae.
These nutrients can be stirred up from the ocean floor due to severe storms. Runoff from fertilizers after heavy rains is another culprit. The severity of red tides depends on the availability of nutrients, the amount of salt in the water, the temperature and wind speed and direction.
The problem with red tides is that they can be toxic. In some aquatic species, the toxins from red tides can cause disruption in nerve signals. The algae also depletes oxygen levels in the water. Both of these occurrences can be deadly to ocean species.
In humans, the toxins from red tides can be inhaled, ingested or absorbed through the skin. Some shellfish and drinking water can become unsafe to consume. Swimming is allowed. But if you suffer from certain conditions, it is best to stay out of the water. And if your skin or eyes become irritated while swimming, get out immediately.
Those who have compromised respiratory health or suffer from chronic conditions should avoid the wate, as toxins from the red tide can make breathing difficult. Also, those who are prone to allergies or skin irritation should use caution as burning of the eyes and rashes on the skin can occur.
If you are traveling to a beach a short distance from here, there is no need to worry about red tides. But if you are going on vacation to Florida this summer, make sure to stay on top of the beach forecasts.
Hepatitis
Hepatitis is one of the more serious conditions one can get at the beach. Luckily, it is an uncommon occurrence.
Hepatitis in all its forms inflames the liver and, in the worst case scenario, can lead to cirrhosis or cancer. Hepatitis is transmitted through the blood or feces of an infected person. Hepatitis is more likely to be caught in waters that are heavily contaminated with sewage runoff. Still, conditions would have to be just right for a swimmer to contract hepatitis in a large body of salty water.
Flesh-Eating Bacteria
The most terrifying of all illnesses caught at the beach is the dreaded flesh-eating disease. However, it has been around for centuries, even being documented by Hippocrates five centuries before Christ.
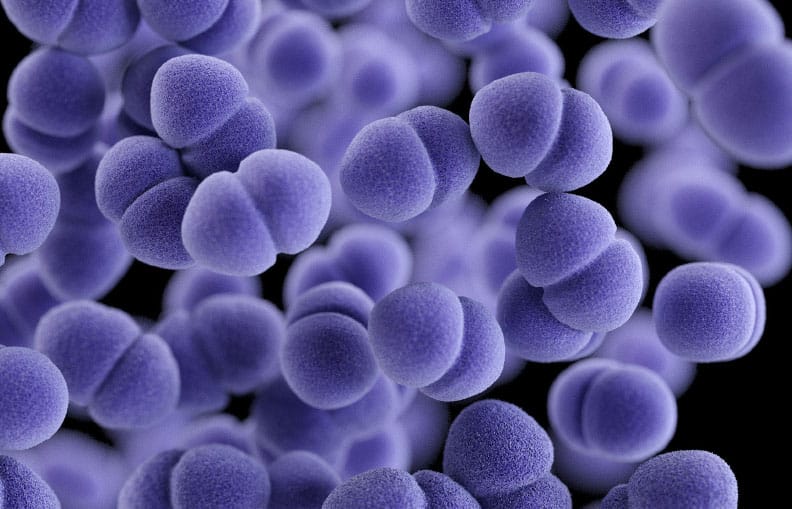
Flesh-eating disease is linked to a few different strains of bacteria, the most common being A Streptococcus.
In simple terms, these bacteria are the same kind that cause strep throat. But what causes common bacteria to become deadly? The experts still haven’t figured that out.
While you might feel like you are always hearing about one case or another of flesh-eating disease, cases are still rare. And they often happen in individuals who have underlying health issues. If the immune system is weakened, bacteria have an easier time penetrating the body’s natural defense system. Risk factors include cirrhosis, kidney disease, cancer, diabetes and liver disease. Older people are at greater risk, as well. It is not impossible for a healthy person to contract the infection, though.
The most common way to contract flesh-eating disease is through open wounds, such as cuts, insect bites or punctures.
There are some situations in which you might not give an open wound a second thought. For example, what if you recently shaved your legs and got a microscopic cut? What if you are a drug user and regularly stick a needle into your arm?
It can be dangerous to overlook such minute breaks in the skin. But if you want an example, there was a man who contracted flesh-eating disease after going into the water with a fresh tattoo. If you get a cut while in the water or while handling shellfish, be extra vigilant in wound care, as bacteria occur in higher numbers on rock or shell-like surfaces.
Safety tips include not going into the water with an open wound and practicing wound hygiene. Flesh-eating bacteria aren’t exclusively found at the beach since strep bacteria is fairly widespread, so always wash your hands and cuts.
Even if you go into the water with an open wound, that doesn’t mean you will contract flesh-eating disease. Healthy immune systems will usually fight off even serious infections like this one.
Flesh-eating bacteria become dangerous once they make their way past the barrier of the skin. They travel very quickly to the muscles and tissues before entering the bloodstream.
The problem with flesh-eating disease is that early onset can mirror symptoms of many other ailments and the infection must be treated as soon as possible to limit damage. Early treatment is critical in order to mitigate symptoms and prevent loss of limb and life.
Early symptoms after one has contracting flesh-eating disease include red or purple skin near the point of entry, fever, nausea or vomiting, diarrhea, dizziness, intense pain, oozing of fluids from the point of entry, hardening and loss of sensation on the skin. The body can go into shock. Then sepsis and organ failure can occur.

Contracting flesh-eating disease is serious, but the rate of infection is about 0.4 per 100,000 people in the U.S. each year. Rates in western Europe are higher, at 1 person per 100,000.
While the strep bacteria causes most cases of flesh-eating disease, there is another bacteria that can do so. V. Vulnificus is contracted by eating raw, contaminated seafood (remember those warnings on restaurant menus about raw seafood) as well as through open wounds. However, this bacteria doesn’t penetrate into the body as deeply as strep.
Curiously, almost every case of infection with V. Vulnificus involves men. Furthermore, the bacteria seem most common in men over the age of 50. While strep does not discriminate between its victims, it is thought that the gender difference in infection with V. Vulnificus is due to the presence of estrogen in women, which helps ward off infection, and the lower levels of iron in a woman’s body, since bacteria need iron to flourish.
While flesh-eating disease is serious, there’s no major need to worry since it is rare and cases do not seem to be increasing.
But to be safe, make sure you don’t go into ocean water or freshwater with an open wound, clean your wounds thoroughly and avoid those big rocks at the beach, which can be breeding grounds for bacteria. If you do choose to walk on the rocks, make sure and wear sturdy shoes and clean any wounds you may receive immediately. If you get any other cuts at the beach, follow the same procedure.
What About That Beach Trip?
You shouldn’t cancel your beach trip because of illnesses that may or may not happen. Use this as a manual to stay safe and healthy while being a beach bum. Be informed on local conditions, and if you happen to get sick, evaluate your symptoms to see if they warrant a trip to the doctor or simply an oatmeal bath.
There are many illnesses in this world, and they all sound scary when you start analyzing them. But we do not simply stay in our houses all winter because we might catch the flu. So go ahead and have your fun day in the sun.
















Comments are closed.